Dr. Karen Horton has either authored or reviewed and approved this content.
Page Updated:
In recent years, fat transfer procedures have become a trusted tool in reconstructive surgery, particularly for secondary breast revision or minor outpatient touch-up procedures. By using fat from your own body, Dr. Horton can achieve further enhancement of natural-looking results that support both breast rejuvenation and improved body contouring.
At her San Francisco Plastic Surgery practice, Dr. Karen Horton offers fat grafting to the breasts—also known as “lipo-filling”—as part of advanced breast reconstruction procedures.1 Serving patients throughout the Bay Area, Dr. Horton uses this technique to refine breast shape, correct asymmetry, and enhance outcomes in secondary breast revision surgeries.
Please note: Our office is no longer a Participating Provider for insurance. After your consultation, we can provide a financial quote for the anticipated surgical fees.
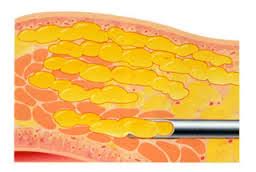 Fat grafting to the breasts involves removing fat cells from one part of the body—typically where there is excess fat, such as the abdomen, thighs, or flanks—and transferring them to the chest as part of a breast reconstruction procedure. The area where the fat is taken from is known as the donor site, a concept also used in free flap techniques during reconstructive surgery.
Fat grafting to the breasts involves removing fat cells from one part of the body—typically where there is excess fat, such as the abdomen, thighs, or flanks—and transferring them to the chest as part of a breast reconstruction procedure. The area where the fat is taken from is known as the donor site, a concept also used in free flap techniques during reconstructive surgery.
Through small, discreet incisions (often hidden in natural folds like the belly button, groin crease, or previous surgical scars), a blunt-tipped cannula is used to perform liposuction and collect fat from the donor site.2 The fat is then gently washed and strained in a sterile environment before being carefully reinjected into the chest to enhance shape, restore volume, or improve contour after reconstruction.
A patient with sufficient fat to harvest for grafting and a recipient site that would likely accept the fat is a candidate for free fat grafting. These individuals are also considered good candidates for liposuction.
If there is not enough fat to harvest, or if the area to be filled requires more than the fat that is available, then fat grafting will not likely be recommended. There are very few contraindications (reasons why fat grafting would not be recommended) for fat grafting.
If you’re considering a fat transfer breast augmentation procedure as part of your reconstructive surgery, proper preparation plays a key role in achieving smooth recovery and natural-looking results.
During your initial consultation at our San Francisco Bay Area practice, Dr. Horton will evaluate your goals, medical history, and current breast appearance, including any asymmetry or changes related to previous surgical procedures. She will also assess potential donor areas where unwanted fat can be safely removed using liposuction. These areas often include the abdomen, thighs, or flanks, and the harvested fat is then purified and prepared for transfer.
To prepare for your fat transfer procedure, patients must maintain a stable weight and avoid significant weight fluctuations. Discontinuing smoking and nicotine use in any form at least six weeks before surgery is required, as nicotine can interfere with healing and fat graft survival. Dr. Horton will provide detailed pre-op instructions and may request updated imaging or after photos for your medical record.
It’s important to have realistic expectations—while fat grafting can offer soft, natural-looking improvement, it is typically used to fine-tune results rather than make dramatic changes in cup size.3
A Note on GLP-1 Medications: If you are currently taking a GLP-1 receptor agonist such as semaglutide or tirzepatide, you must stop taking it at least one month before your tummy tuck surgery. These medications affect gastric motility and anesthesia safety and can negatively influence wound healing after surgery; you will be educated more about these risks and be provided with specific guidance during your consultation. Learn more here.
Fat grafting is typically performed under general anesthesia in a sterile operating room. Dr. Horton begins by marking the donor site, then uses small incisions and a tumescent solution to minimize bruising, bleeding, and post-op discomfort. Excess fat is gently removed via liposuction, collected in a sterile system, and carefully washed—never centrifuged per the fat grafting collection system manufacturer’s recommendations—to preserve fat cell integrity.

Multiple small syringes are filled with processed fat before reinjecting it into its new location in the chest area.
While the patient is still asleep, the harvested fat is transferred into small syringes and precisely injected into the chest area through tiny incisions. This technique is used to correct asymmetry, fill hollows, or reduce implant rippling for a more natural-looking result. The incisions are closed with dissolvable sutures, and a compression garment—such as an ACE wrap, abdominal binder, or traditional post-liposuction compression garment—is applied before the patient awakens.
Fat grafting is performed as an outpatient procedure. Patients may choose to stay overnight in a hotel close to our surgery center before traveling home if additional surgeries are performed at once or they’re traveling from outside the Bay Area.
After a fat grafting procedure, patients usually go home the same day and are seen back in the office within a week. Bruising is expected for at least a few weeks, and exercise can resume within around three weeks, or when discomfort resolves. Sutures dissolve on their own, and the postoperative compression garment can be discontinued when the bruising goes away, or per the patient’s comfort. Numbness of the area where fat was harvested is expected for several weeks, and potentially up to a few months, as the sensory nerves to the skin recover, just like other types of surgery.

Liposuction canisters filled with fat after a cosmetic liposuction case. The same amount of fat is often removed in free fat graft harvest, which serves as a bonus to the patient!
Following fat grafting, firm swelling called “edema” can persist for several months after surgery, particularly in dependent areas most affected by gravity. At around three months, we can expect to see the final results of the fat grafting – i.e. how much fat survived in the recipient area and the new contour of the donor site. It can take up to a full year for ALL post-surgical swelling to go down in the donor sites. Numbness in the operated area is temporary, and postoperative discomfort is usually minimal. See our section on cosmetic liposuction recovery for additional information about recovery after free fat graft harvest.
Can Fat Grafting Create an Entire Breast Starting from a Flat Post-Mastectomy Chest?
Unfortunately, no. It is necessary for a breast mound to already be present for a patient to wear an external suction-based expander device, and by the description, you can imagine that it is not likely comfortable, fun, or user-friendly at all to wear! Even if the external suction device was worn religiously for the recommended time, a very thin mastectomy skin flap would not be expected to expand its volume so much that fat graft take would be significantly improved.
The predicament for the slender, thin-skinned breast reconstruction patient, where the recipient site cannot accept a significant amount of fat, remains the same. It is difficult to inject a great deal of fat into a thin, unhealthy, or radiated area.
See a recent blog post on free fat grafting to the breast to learn even more. The only solution in this situation (very thin chest skin after mastectomy or lumpectomy, radiation, infections or complications, implant rippling or an unsatisfactory breast reconstruction) would be to perform a free flap reconstruction using abdominal tissue or inner thigh tissue, and to bring additional healthy, thicker tissue to the chest area using Microsurgery.
What Is the Difference Between a Fat Graft and a Flap?
The free-floating fat cells, after being removed from the body, have lost their blood supply and are free-floating hence the term “FREE fat grafting”. As opposed to a free flap, which carries its blood supply via small arteries and veins that are disconnected and then reconnected using Microsurgery, a free fat graft does not have an attached blood supply, and the cells are therefore called a GRAFT (no associated blood supply) as opposed to a FLAP (which comes with a blood supply).
Commercial fat graft collection systems allow fat cells to remain sterile and be gently washed and concentrated before being injected into the body.
After processing of the fat while the patient is still asleep, the fat cells are injected into a new part of the body, – for instance, into a hollow or contour depression at the top of the chest, either resulting from a mastectomy or related to a congenital condition such as Poland Syndrome.
When the fat cells are injected into their new location, it is anticipated that some fat cells will acquire a new blood supply from the surrounding recipient site and remain in that location. However, after fat grafting, regardless of the skill of the surgeon or gentleness of the technique, we can only expect around 30% of the fat cells to find a new blood supply and successfully survive in their new location. This is called "the free fat graft take”, or fat cell survival.
The process of transplanted fat cells’ survival is very different from what happens with a free flap such as the DIEP flap or the TUG flap in which a segment of structural tissue (skin and fat with all the anatomic connections) carries its own internal circulatory system with it to its recipient site, and where blood vessels are reconnected under the microscope to ensure the flap survives as a whole in its new location.
Why Can’t Fat Grafting Be Used to Reconstruct the Entire Breast?
With a Microsurgical free tissue transplantation (free flap) such as the DIEP flap, SIEA flap or TUG flap, it is expected the fat cells will survive up to 100%, with only very small peripheral areas getting the least blood supply (and resulting in discrete hard areas of firm fat, called “fat necrosis”). This is why a free flap is used for the primary breast reconstruction, and free fat grafting only for small touch-ups afterward. It would be very time-consuming and extremely inefficient to attempt to build an entire breast reconstruction using only fat grafting as the primary method!
What Happens to the Fat Cells that Don’t Survive?
Since only around 30% of the transplanted fat cells can be expected to “take” in the recipient site, that means up to 70% of the fat cells will, in turn, not survive and be absorbed, to our dismay. The body naturally clears fat cells that don’t survive, just as when normal fat cells reach their lifespan, expire, and turn over elsewhere in the body through natural processes —this is called programmed cell death, or “apoptosis”. In order to account for the small amount of fat graft survival, the area is over-filled (if possible) to take into account for partial “take” expected after fat grafting.
Can Anything Be Done to Improve Fat Graft Take?
There is an external expansion system that some surgeons use for their patients called the BRAVA device. This process involves wearing a contraption on the chest that essentially is two suction cups attached to a machine that sucks the breast tissue into the cups at least 10 hours a day for several weeks to months before fat grafting is performed. The theory is that the suction will increase blood flow to the breasts and potentially improve the survival of fat cells with grafting.
Incredibly, some women are willing to commit to this machine in the hopes that the suction will increase circulation to the area, increase the volume of tissue that may accept an implant, and improve free fat graft cell survival. Research is ongoing in this area, and most Plastic Surgeons who perform breast reconstruction have not incorporated this device into their practices.
How Much Fat Is Typically Removed in a Fat Grafting Procedure?
Generally, as much as possible! Visit our blog to see an image of how much fat can be removed after liposuction. The process of fat graft harvest is nearly identical for free fat grafting, but the fat is washed and reinjected into the recipient site rather than discarded.
Liposuction canisters are filled with fat after a cosmetic liposuction case. The same amount of fat is often removed in free fat graft harvest, which serves as a bonus to the patient!
Can Fat Grafting Fix Rippling or “Wrinkling” of an Implant?
An implant is visible under the skin for one reason —lack of padding or soft tissue coverage, also known as very thin skin over the implant. This occurs either because a woman is naturally thin in the chest area or because an aggressive mastectomy created very thin coverage for the implant.
Regardless of whether an implant is under the muscle or not —such as in immediate single-stage breast implant reconstruction we offer to patients —if a woman has extremely little subcutaneous fat, or if the mastectomy surgeon removed so much of the fat in the area of surgery, an implant might be visible through the skin. This is known as breast implant “rippling” or “wrinkling”, and it is a frustrating problem to correct.
Fat grafting to the area can somewhat improve the appearance of rippling in this situation; however, there needs to be sufficient tissue thickness in the area to accept a significant amount of fat graft cells. I often describe the situation as “trying to inject a piece of paper with a cup of water”; the thin paper is not very absorbent, and no matter how hard we try, the paper will not accept much, as opposed to conceptualizing injecting a thick sponge full of the same amount of water. We can always attempt a session of free fat grafting in order to improve implant rippling, but the results may not be as dramatic or successful as we might hope for this situation.
What Else Can Be Done to Correct or Improve Breast Implant Rippling?
In the United States, there are a variety of recently introduced options to help correct breast implant rippling, including new styles of fuller volume breast implants and other mesh-like products that can be added to improve the support of the implant in its space. However, with very thin post-mastectomy skin and lack of padding over the implant, even the very best breast reconstruction can still have some rippling —this is a sign that the implant is soft, there is no capsular contracture, and the patient is thin over the implant!
What Are the Potential Risks and Complications of Fat Grafting?
See my website page on liposuction to learn more about risks and potential complications of fat graft harvest, which are the same as for cosmetic liposuction. When the fat graft is injected, it must be distributed evenly through the recipient site. If too much fat is injected in one area, it is possible that none of it may survive, and an oil cyst or area of firm fat necrosis (hard, dead fat) may be created.
While we expect at least 30% of the fat cells to survive, it is possible that none of the fat could take up a new blood supply, and it could all go away (although this is rare). Conversely, some patients have a much better survival of fat graft cells, in the range of 50-70% or more. However, these patients usually have a healthy, thick recipient site that readily accepts the fat graft, such as a free flap breast reconstruction or healthy, thick tissue that is not radiated or many scars.
When Will Fat Grafting Be Recommended as Part of My Breast Reconstruction Procedure?
Free fat grafting is usually incorporated into a secondary or “touch-up” procedure after a primary breast reconstruction with a breast implant or a flap. Fat grafting is also becoming routine as a component of revision breast surgery after an initial breast reconstruction procedure following mastectomy. I usually do NOT recommend that a natural breast or one that still has breast tissue present (and that will be undergoing mammograms in the future) have fat grafting performed.
Can Fat Grafting Be Used to Augment My Breasts? Isn’t This “Natural Breast Augmentation”?
While it IS possible to add fat to a natural breast, I feel very strongly that doing so can hinder breast cancer detection and mammogram screening, and I usually recommend AGAINST it. Read my blog post on fat grafting to a natural breast to learn more and to fully understand this complex and somewhat controversial issue.
What Happens If You Gain Weight After Fat Grafting?
This is an excellent question! Interestingly, we are only born with a certain number of fat cells, and when they are removed using
liposuction, these fat cells are gone forever! As long as you maintain a healthy lifestyle and consistent weight, results at the donor site after liposuction or a free fat graft harvest are permanent. Read my educational blog posts about liposuction, which go into additional detail about weight changes after liposuction and expected changes with weight gain and weight loss.
However, when we perform free fat grafting, we save those stubborn fat cells that persist despite diet, exercise, and our best efforts, and instead of discarding them, we transplant them to a new location where many of them will survive. In the case of fat grafting to fill in a hollow or contour depression resulting from breast cancer surgery, the result in the recipient site after weight gain could be positive and even beneficial!
Weight gain could theoretically improve the contour of the area to which the fat was injected in the chest after free fat grafting for breast reconstruction. Weight loss could, in turn, cause all fat cells to shrink, including the fat that was transplanted to the chest, with a general loss of fat everywhere. In reality, most people do not have extreme swings in their weight, and results tend to be relatively consistent over time.
Can Fat Grafting Be Done to Other Areas of My Body?
Yes, it is possible to graft fat to nearly any area of the body where augmentation is desired. This includes the buttocks, chest, calves, face, under-eye area, lips, and even the backs of the hands, where age-related changes are often apparent.
Why would anyone want to have fat grafting in these areas? For the same reason that you would consider augmenting the breasts and buttocks, or have dermal filler injected to add volume or conceal thin, aging skin, free fat grafting can be done to other areas. Keep in mind that the same caveats exist – there must be enough fat to harvest from a donor site in the body, the recipient site must be thick and healthy enough to accept the fat cells, and we can only expect around 30% (on average) of the fat cells to survive. Many patients feel it is a lot of work for very little gain, especially if it is a cosmetic procedure. For this reason, injectable dermal fillers are very popular, especially in my office with an experienced injector such as Emily Sespaniak, NP!
More About Fat Grafting to the Face and Other Areas
I CAUTION patients to beware and be careful about having fat injected into their face, particularly if they are young, have not yet had children, and their weight may increase in the future.
Unfortunately, at some of my professional society meetings, entire expert panels are starting to be dedicated to discussing this exact problem —correcting monstrous deformities resulting from careless fat grafting to the face, cheeks, lips and buttocks (you name it and it’s been done), and with weight gain and changes of aging, patients look strange and even deformed!
“Fringe medicine” procedures, such as careless fat grafting to young people’s faces, are increasingly being offered by “cosmetic doctors” who are not Plastic Surgeons and are often not Board Certified by the American Board of Plastic Surgery.
Fat grafting to the face is generally not recommended by Board Certified Plastic Surgeons as a primary filling technique when dermal fillers have not yet been tried. Why? It is very difficult to remove fat from the face or under the delicate skin of the face because large quantities of fat are not normally stored there, and liposuction is not normally done in these locations. DO YOUR HOMEWORK!
If a patient is a candidate for augmentation to the face, I recommend dermal filler injections. Most dermal fillers are long-lasting (six months up to two years or longer), but can also be reversible by way of injecting an enzyme that will dissolve the product if the results are no longer wanted.
What Are the Take-Away Messages About Free Fat Grafting?
To summarize, free fat grafting is a wonderful adjunct to breast reconstruction after mastectomy for breast cancer or for Poland Syndrome chest wall reconstruction. The results are not magic, but can achieve a subtle improvement in the recipient site. In many cases, the biggest benefit is to the donor site, as we can contour the abdomen, hips, inner and outer thighs or flanks at the same time as improving the results of breast reconstruction.
What Does the Future Hold for Free Fat Grafting?
The future of fat grafting probably involves tissue engineering and 3D printing! I envision that stem cells harvested by liposuction and a three-dimensional construct grown in the laboratory that exactly matches the breast size, shape, and dimensions desired by a patient will be possible. It is exciting to imagine how the technology of 3D printing and human biologic tissue engineering can be used to build a breast, and how Microsurgery can then transplant the tissue construct into the body. Exciting possibilities!
Until then, my office offers the latest techniques available for aesthetic reconstruction for women who are facing breast cancer or hereditary increased risk of cancer and are seeking mastectomy.
1 BreastCancer.org. Fat Grafting. https://www.breastcancer.org/treatment/surgery/breast-reconstruction/types/autologous-flap/fat-grafting. Accessed May 21, 2025.
2 Cleveland Clinic. Fat Transfer Breast Augmentation. https://my.clevelandclinic.org/health/treatments/24033-fat-transfer-breast-augmentation. Accessed May 21, 2025.
3 American Society of Plastic Surgeons. Fat Transfer Breast Augmentation. https://www.plasticsurgery.org/cosmetic-procedures/fat-transfer-breast-augmentation. Accessed May 21, 2025.
Dr. Karen Horton has either authored or reviewed and approved this content.
Give us a call or fill out form below to schedule online.
Monday-Friday: 9am - 5pm
Saturday-Sunday: Closed
Monday:
9 AM to 5 PM
Tuesday:
9 AM to 5 PM
Wednesday:
9 AM to 5 PM
Thursday:
9 AM to 5 PM
Friday:
9 AM to 5 PM
Saturday:
Closed
Sunday:
Closed
Dr. Karen M. Horton
2100 Webster St., Suite 520
San Francisco, CA 94115
Phone: 415.923.3067
We are located in the
Pacific Heights District
in the Pacific Professional Building.
 SHOP SKIN CARE
SHOP SKIN CARE*Please note: Our office is no longer a Participating Provider for insurance. We can provide a financial quote for what anticipated surgical fees will be after your consultation.